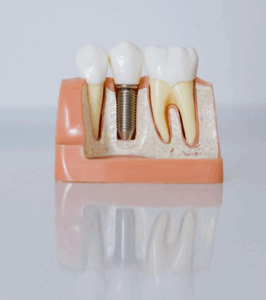
Single tooth implants represent a critical restorative option in modern dentistry for addressing the gap left by a missing tooth. The procedure involves placing a titanium post into the jawbone, which serves as a root substitute, providing stability for the prosthetic tooth. This method is particularly advantageous when adjacent teeth remain healthy, preserving their integrity. Extensive evaluation of gum health, bone density, and overall oral condition is essential, prompting further exploration into its candidacy and procedural intricacies.
Understanding Single Tooth Implants
How do single tooth implants in Long Beach function as a solution for missing teeth? These implants serve as an effective prosthetic intervention by mimicking a natural tooth’s structure and function. Surgically inserted into the jawbone, they provide a stable anchor for an artificial crown. This process not only restores the cosmetic appearance but also maintains the overall tooth alignment. By filling the gap left by a missing tooth, implants prevent adjacent teeth from shifting, which could otherwise lead to malocclusion or bite issues. The osseointegration process, where the implant merges with the bone, guarantees durability and functional harmony with surrounding oral structures. Consequently, single tooth implants offer a reliable option for both functional restoration and aesthetic enhancement in dental treatment.
Assessing the Health of Surrounding Teeth
Before proceeding with a single tooth implant, evaluating the health of surrounding teeth is imperative to guarantee a successful outcome. Clinicians must conduct a thorough assessment focusing on tooth mobility, as increased mobility can indicate compromised periodontal support, which might affect implant stability. Radiographic evaluations are essential to identify any previous root canal treatment, which can be indicative of underlying pathological conditions. Teeth adjacent to the implant site should be scrutinized for structural integrity, caries, and any signs of endodontic failure that could necessitate further intervention. An interdisciplinary approach may be required, involving endodontists to address potential issues with root canal-treated teeth. By ensuring adjacent teeth are healthy and stable, practitioners can substantially enhance the prognosis of the implant procedure.
Evaluating Gum Health and Bone Density
Evaluating the suitability of a single tooth implant necessitates a thorough assessment of gum tissue condition and bone density. Clinicians must analyze the integrity of the jawbone structure using diagnostic imaging to guarantee adequate support for the implant. Determining bone density levels is critical to predict the long-term success and stability of the implant within the oral cavity.
Assessing Gum Tissue Condition
When determining the suitability of a single tooth implant, the condition of the gum tissue serves as a pivotal factor. Clinicians perform a thorough assessment focusing on several key areas:
- Evaluating Pocket Depth: Measuring the depth of the gingival sulcus is essential to identify periodontal health. Deep pockets may indicate periodontal disease, complicating implant placement.
- Monitoring Gum Recession: Observing gum recession is paramount, as it can affect the stability and aesthetic outcome of the implant. Recession should be minimal to guarantee adequate support.
- Assessing Inflammation: Identifying signs of inflammation, such as redness or swelling, is indispensable. Inflammation can compromise healing and implant success.
- Checking Tissue Biotype: The thickness and quality of the gum tissue impact implant integration and aesthetics. A thicker biotype is generally more advantageous.
Analyzing Jawbone Structure
Following the assessment of gum tissue, an in-depth evaluation of the jawbone structure becomes paramount in determining the feasibility of a single tooth implant. A thorough jawbone structure assessment involves radiographic imaging techniques such as panoramic radiographs or CBCT scans to visualize the bone’s architecture. Clinicians conduct a bone density analysis to ascertain the quality and volume of the existing alveolar bone, which is critical to implant stability. This procedural focus guarantees that the jawbone can adequately support the implant fixture and withstand occlusal forces over time. Additionally, identifying any anatomical irregularities or pathologies within the jawbone structure informs the surgical planning process. Such evaluations are integral to formulating a treatment plan that optimizes implant success rates and long-term functionality.
Determining Bone Density Levels
In evaluating the suitability for a single tooth implant, determining bone density levels is a crucial step that complements the assessment of gum health. Bone quality assessment safeguards the structural integrity necessary for implant success. Radiographic analysis serves as a pivotal diagnostic tool, providing detailed images for evaluating osseous architecture. The procedure typically includes the following steps:
- Radiographic Analysis: Utilizes advanced imaging techniques such as Cone Beam Computed Tomography (CBCT) to assess bone volume and density.
- Bone Quality Assessment: Classifies bone into types (D1-D4) based on density and trabecular pattern.
- Clinical Examination: Inspects oral cavity for signs of periodontal disease impacting bone health.
- Evaluation of Systemic Factors: Reviews patient history for conditions affecting bone metabolism.
This complete approach guarantees optimal implant placement and longevity.
Considering the Impact on Oral Function
Although single tooth implants are commonly chosen for their aesthetic appeal, their impact on oral function is equally significant. Clinically, these implants play a vital role in restoring optimal bite function, which is paramount for effective mastication and overall dental health. The absence of a tooth can lead to maladaptive speech patterns due to the disruption of the oral cavity’s natural anatomy. By reinstating a proper occlusal relationship, single tooth implants facilitate improved articulation and prevent potential speech impediments. Furthermore, they offer stability and support to adjacent teeth, thereby maintaining occlusal harmony. The procedural focus on accurately placing implants guarantees that they mimic the natural tooth structure, which is essential in preserving the functional integrity of the patient’s dentition.
Weighing Aesthetic Concerns
Aesthetic considerations play a pivotal role in the decision-making process for single tooth implants, particularly in visible areas of the mouth. These considerations often emphasize the personal image impact and social confidence boost that can be achieved. Clinicians evaluate several factors to optimize aesthetic outcomes:
- Shade Matching: Ensuring the implant crown matches the natural teeth in color is essential for seamless integration.
- Gingival Architecture: The contour and health of the surrounding gum tissue are critical for a natural appearance.
- Tooth Morphology: The shape and size of the implant crown must replicate the natural tooth to maintain harmony in the dental arch.
- Material Choice: Selecting biocompatible materials enhances aesthetic longevity and mimics the translucency of natural teeth.
These components collectively contribute to the overall visual success of the implant procedure.
Reviewing Long-Term Oral Health Benefits
Single tooth implants offer substantial long-term oral health benefits, particularly in the prevention of alveolar bone resorption. By providing necessary stimulation to the jawbone, these implants help maintain structural integrity and prevent the detrimental effects of bone atrophy associated with tooth loss. Consequently, the preservation of oral architecture is effectively supported, which is essential for overall dental functionality and aesthetics.
Prevents Bone Loss
How do dental implants contribute to preventing bone loss in patients with missing teeth? Dental implants are vital due to their ability to maintain oral integrity and prevent further tooth loss. The osseointegration process, wherein the implant fuses with the jawbone, is pivotal. This fusion simulates natural tooth roots, offering the following benefits:
- Stimulates Bone Growth: Implants provide necessary mechanical loading, encouraging osteoblastic activity.
- Reduces Bone Resorption: By replacing the lost tooth root, implants inhibit the bone resorption process.
- Maintains Jawbone Density: The continuous stimulation of the jawbone helps in preserving its density and structure.
- Enhances Periodontal Health: By maintaining the position of adjacent teeth, implants contribute to overall periodontal stability.
Through these mechanisms, dental implants effectively avert bone deterioration.
Maintains Oral Structure
Following the prevention of bone loss, dental implants play a significant role in maintaining oral structure, which is integral to long-term oral health. The structural integrity of the jaw is essential for sustaining facial aesthetics and functionality. Implants serve as artificial roots, supporting the osseointegration process that maintains facial structure. This foundation prevents adjacent teeth from migrating, thereby preserving natural tooth alignment. Such stabilization minimizes occlusal disharmony, which can lead to further oral complications. Clinically, single tooth implants are preferred as they mitigate the mesial drift and tilting often observed with missing teeth. This procedural intervention effectively circumvents the cascade of misalignments and periodontal issues. As a result, dental implants are indispensable in ensuring the preservation of dental and facial architecture.
Analyzing Lifestyle and Habits
Understanding the impact of lifestyle and habits on oral health is crucial when considering single tooth implants for missing teeth. Key factors include personal hygiene habits and dietary preferences, which can drastically influence implant success. A clinical evaluation should assess the following:
- Oral Hygiene: Adequate personal hygiene habits, including regular brushing and flossing, are indispensable to mitigate peri-implantitis risk.
- Dietary Habits: High sugar and acidic diets may compromise implant longevity due to increased plaque.
- Tobacco Use: Smoking is a well-documented risk factor, negatively impacting osseointegration and implant stability.
- Alcohol Consumption: Excessive alcohol can impede healing and should be discussed during pre-implant consultations.
Financial Considerations and Insurance Options
In evaluating the financial implications of single tooth implants, a cost comparison analysis is essential, contrasting implant expenses with alternative tooth replacement methods. Insurance coverage details should be meticulously reviewed, as policies vary with respect to procedures covered and reimbursement rates. Additionally, exploring available payment plan options can assist patients in managing out-of-pocket expenditures efficiently.
Cost Comparison Analysis
Evaluating the financial implications of single tooth implants requires a detailed analysis of both direct costs and potential insurance coverage. An ideal cost estimate breakdown includes several components:
- Implant Component Costs: This involves the titanium post, abutment, and crown. Material selection may influence overall expenses.
- Procedural Fees: Surgical and prosthetic procedures necessitate professional fees, which can vary depending on clinical expertise and geographic location.
- Ancillary Expenses: These may encompass diagnostic imaging, anesthesia, and any necessary bone grafting for optimal implant stability.
- Projected Treatment Duration: Time required from initial consultation to final restoration can impact cumulative costs, with longer timelines possibly accruing additional follow-up visits.
Understanding these variables aids in formulating a strategic financial plan for implant therapy.
Insurance Coverage Details
Traversing insurance coverage for single tooth implants involves evaluating a multitude of factors that can drastically impact financial outlays. The primary consideration is the insurance premium costs associated with dental plans offering implant coverage. Not all insurance policies encompass dental implants, as they are sometimes classified under cosmetic procedures, thus consequently falling outside standard coverage. Consequently, potential patients must scrutinize insurance plan limitations that dictate the extent of coverage for restorative dental work. Some plans may offer partial reimbursement, while others might exclude implant procedures entirely. Evaluating the specifics of each policy, including annual maximums and co-payment structures, is crucial. Understanding these variables allows individuals to assess the economic feasibility of pursuing a single tooth implant under their current insurance framework, ensuring informed financial decisions.
Payment Plan Options
When considering single tooth implants, patients often explore various payment plan options to manage financial obligations efficiently. Financing options vary, and understanding payment plan details can profoundly impact the decision-making process. Clinicians typically provide structured payment plans that align with typical treatment phases.
- Interest-Free Installments: Patients may opt for monthly payments over a defined period without incurring interest, facilitating manageable budgeting.
- Extended Payment Plans: Longer-term financing with interest, suitable for those needing lower monthly payments.
- Third-Party Financing: Collaborations with financial institutions offering specialized healthcare credit plans.
- Insurance Integration: Coordinating with dental insurance to cover partial expenses, reducing out-of-pocket costs.
Each option requires careful consideration of the patient’s financial capacity and the procedural cost of implant treatment.
Timing After Tooth Extraction
Following a tooth extraction, the timing of a single tooth implant is a critical consideration in clinical practice. Determining the ideal timing for implant placement involves evaluating the patient’s oral health and bone healing status. An appropriate waiting period, typically ranging from immediate placement to several months post-extraction, allows for optimal osseointegration and gingival tissue stabilization. Immediate implant placement can be advantageous, guaranteeing preservation of the alveolar ridge and reducing treatment time. However, this approach may not be suitable for all patients, especially those with infections or insufficient bone density. Delayed implant placement, after a healing period of 3-6 months, is often recommended to enable complete bone remodeling and guarantee implant stability. Clinicians must carefully assess these factors to optimize procedural outcomes.
Consulting With a Dental Professional
Consultation with a dental professional is an essential step in the process of obtaining a single tooth implant. It involves a systematic evaluation to guarantee clinical suitability and to align expectations of the patient with procedural outcomes. During these consultations, the dental professional will:
- Assess Oral Health: Analyze the patient’s oral and systemic health to confirm candidacy for the implant procedure.
- Review Imaging: Utilize radiographic imaging to evaluate bone density and anatomical structures vital for implant placement.
- Discuss Qualifications: Present their credentials, experience, and success rates in performing single tooth implants to build patient confidence.
- Explain Procedure: Detail the procedural steps, potential complications, and post-operative care, making sure the patient comprehends the process.
This structured consultation enables informed decision-making and sets a realistic framework for treatment success.
Frequently Asked Questions
What Is the Success Rate of Single Tooth Implants?
The success rate of single tooth implants is high, with implant longevity often exceeding 10 years. Implant failure rates are low, typically ranging between 1-5%, depending on factors like bone quality, surgical technique, and patient health.
Can Single Tooth Implants Cause Allergic Reactions?
Single tooth implants may trigger allergic reactions due to potential material sensitivities. Immune system complications can arise if the body reacts adversely to components like titanium or alloys, necessitating thorough pre-procedural assessments to mitigate such risks.
How Long Does the Implant Procedure Take From Start to Finish?
The procedure duration for a single tooth implant typically ranges from 30 to 60 minutes per session. The overall implant integration timeline, including osseointegration and abutment placement, spans approximately three to six months for successful completion.
Are There Any Dietary Restrictions After Getting a Single Tooth Implant?
After a single tooth implant, patients must adhere to specific dietary restrictions. Maintenance requirements include avoiding hard or sticky foods initially to guarantee proper healing, while chewing considerations involve gradually reintroducing normal diet as guided by clinical evaluation.
Can Single Tooth Implants Be Done for Children or Teenagers?
Single tooth implants in children or teenagers require careful evaluation of tooth development considerations and skeletal maturity concerns. Implantation procedures typically await complete craniofacial growth to guarantee long-term stability and integration, often postponing until post-adolescent skeletal maturity.





